
What to expect after the birth of your baby?
Congratulations on the birth of your beautiful new baby!
You have delivered a baby into the world and now you, as a new mum need care and attention to help you recover, both physically and emotionally from your pregnancy and birth journey.
Signs and symptoms?
- Do you have sore, red and inflamed breasts due to breastfeeding or mastitis (inflammation of the milk ducts)?
- Do you need advice on your C-section scar healing?
- Are you experiencing increased stomach muscle separation (DRAM)?
- Do you need advice on when you should return to exercise?
- Is your bladder or bowel function not returning to normal?
- Are you experiencing pain and changes in your feet or your thumbs?
Common health concerns new mama's experience?
- Sore, red and inflamed breasts or nipples related to breastfeeding or mastitis
- C-section scars and wound care
- Back, sacroiliac joint, pubic symphysis, coccyx, neck and wrist pain
- Stomach muscle separation (DRAM)
- Pelvic floor muscle weakness/overactivity
- Fatigue/lack of sleep, anxiety, mood changes and depression
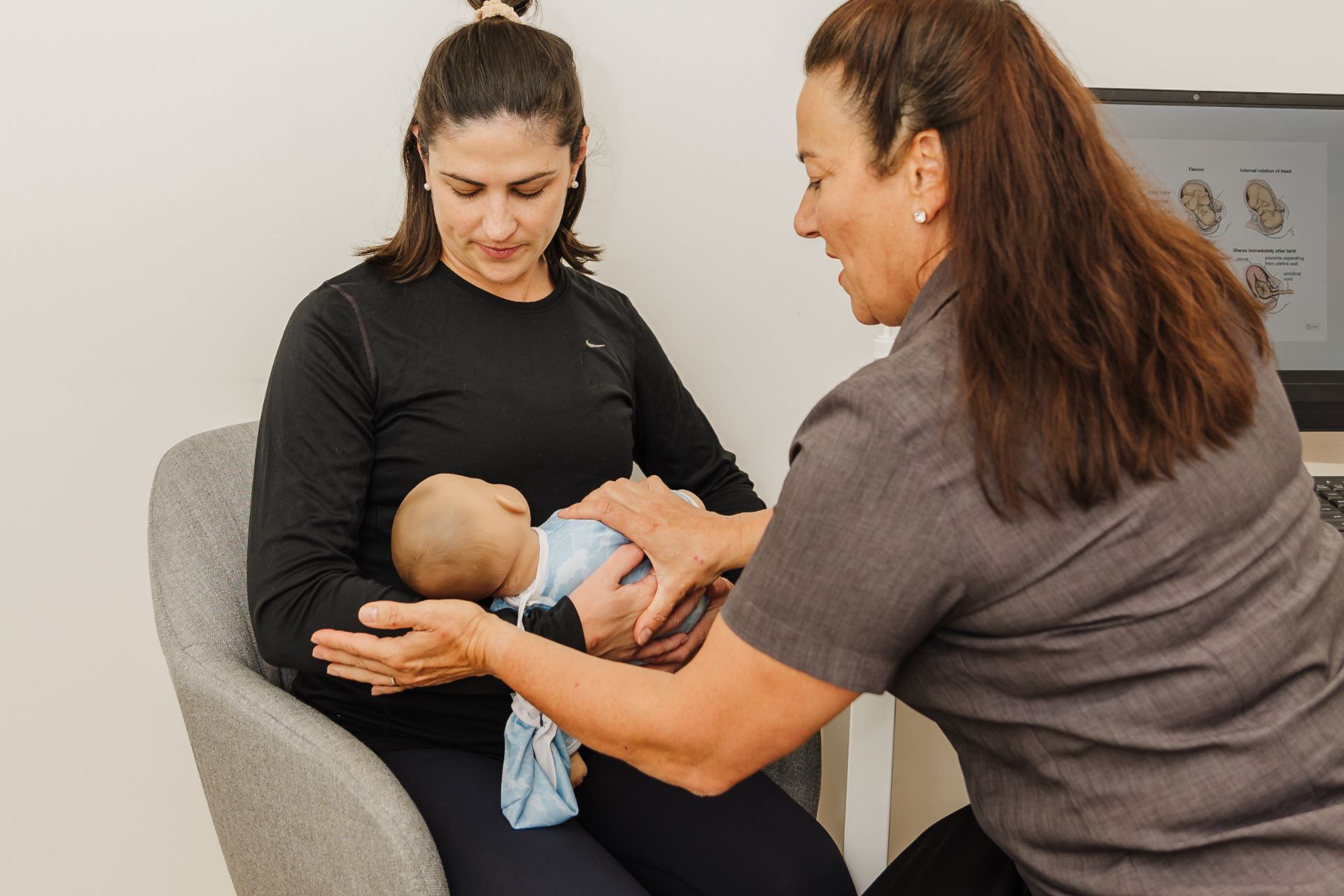
How can we help?
Physiotherapy for a new mama's body recovery?
Physiotherapy treatments for new mums may include:
- Breast and nipple care and treatments for mastitis include massage, therapeutic ultrasound and/or laser therapy.
- Strategies on how to get enough sleep and support for any mood concerns
- C-scar wound management to promote healing using ultrasound, massage and taping supports
- Stomach checks for muscle stretching and abdominal muscle recovery
- Treatment and advice on exercises for back, neck, sacroiliac joint, pubic symphysis, coccyx, hip and wrist pain
- Pelvic floor muscle and vulval skin assessment and rehabilitation program
- Advice on compression garments to assist healing after birth
- Safe return to exercise with an individualised program developed for you
Our team can assist with a postnatal assessment and provide advice and treatment for any concerns you may have.
Related Blogs













